Restoring Skin Health in Patients with Venous Ulcers
Introduction
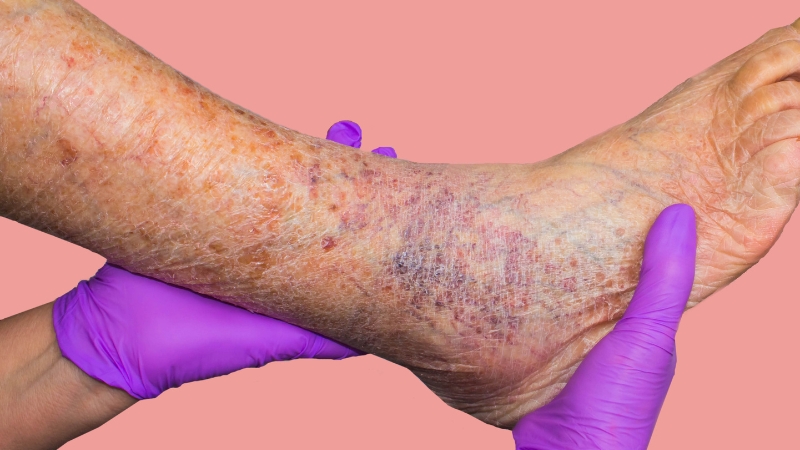
Venous ulcers are one of the most advanced complications of chronic vein disease. These slow-healing wounds typically develop around the ankles and lower legs and can cause persistent pain, swelling, skin discoloration, and recurrent infections. If not treated properly, they may significantly affect mobility, work productivity, and overall quality of life.
Modern vascular care focuses not only on healing the wound but also on identifying and correcting the underlying venous insufficiency responsible for the condition. Early diagnosis and specialized treatment play a critical role in achieving long-term recovery and preventing recurrence.
What Is a Venous Ulcer?
A venous ulcer is an open sore that develops due to improper blood circulation in the leg veins. When vein valves become weak or damaged, blood flows backward and pools in the lower limbs. This condition, known as chronic venous insufficiency, increases pressure inside the veins and eventually leads to skin breakdown.
Venous ulcers most commonly appear near the inner ankle. They may begin as discolored, itchy, or thickened skin before progressing into a painful open wound that heals very slowly.
Common Causes and Risk Factors
- Long-standing varicose veins
- History of deep vein thrombosis (DVT)
- Obesity
- Prolonged standing or sedentary lifestyle
- Aging
- Family history of vein disorders
Individuals with untreated vein disease are at a significantly higher risk. Addressing venous problems early can prevent complications such as chronic wounds.
Recognizing Symptoms Early
Venous ulcers typically develop gradually. Warning signs may include:
- Persistent leg swelling
- Darkening or thickening of the skin around the ankle
- A feeling of heaviness in the legs
- Itching or burning sensation
- Fluid discharge from a wound
If a leg wound does not heal within two weeks, medical consultation is strongly recommended. Delayed care may lead to infection or enlargement of the ulcer.
Diagnostic Evaluation
Accurate diagnosis is crucial for effective treatment. A vascular specialist typically performs a detailed assessment to determine both the severity of the ulcer and the underlying venous condition.
Clinical Examination
A thorough physical examination includes evaluation of swelling, skin texture, discoloration, wound depth, and surrounding tissue condition. The specialist also reviews medical history, previous vein issues, lifestyle factors, and any history of blood clots. This step helps identify contributing causes and assess the stage of chronic venous insufficiency.
Doppler Ultrasound
A Doppler ultrasound is a non-invasive imaging test used to evaluate blood flow in the leg veins. It helps detect valve dysfunction, reflux (backward blood flow), vein obstruction, or clots. This diagnostic tool is essential in mapping affected veins and planning appropriate treatment.
This comprehensive evaluation ensures that treatment addresses not only wound healing but also the root vascular problem to prevent recurrence.
Procedures like transurethral resection of the prostate (TURP) are effective but involve hospital stays, anesthesia, and extended recovery. Some surgeries may also affect sexual function or cause bleeding and infection.
Treatment Options for Venous Ulcers
Successful management of venous ulcers requires a combination of wound care and correction of venous insufficiency.
Compression Therapy
Compression stockings or multilayer bandages help improve blood circulation, reduce swelling, and enhance oxygen delivery to tissues. By applying controlled pressure, compression therapy assists in pushing blood back toward the heart. It is often the first line of management and plays a vital role throughout the healing process.
Advanced Wound Care
Proper wound management includes specialized dressings that maintain a moist healing environment, infection control measures, and skin protection strategies. In some cases, debridement (removal of dead tissue) may be required to promote healthy tissue growth. Consistent wound monitoring significantly improves healing outcomes.
Minimally Invasive Vein Procedures
Modern endovascular treatments target the faulty veins responsible for increased pressure. Techniques such as laser therapy, radiofrequency ablation, or embolization seal damaged veins and redirect blood flow to healthy vessels. These procedures are typically performed on a day-care basis, require minimal anesthesia, and allow faster recovery compared to traditional surgery.
Many individuals seeking varicose veins treatment in India benefit from these advanced minimally invasive solutions that treat the underlying vein disease while supporting ulcer healing.
A personalized treatment plan tailored to the patient’s condition ensures optimal healing and significantly reduces recurrence risk.
Healing and Long-Term Prevention
Healing time depends on the size, duration, and severity of the ulcer. With appropriate treatment, many patients experience noticeable improvement within weeks.
Preventive measures include:
- Maintaining a healthy body weight
- Staying physically active
- Elevating legs when resting
- Avoiding prolonged standing
- Wearing prescribed compression garments
- Regular follow-up with a vascular specialist
Long-term vein health management is essential to prevent future ulcers.
Conclusion
Venous ulcers are not merely skin wounds, they are a sign of underlying venous disease. Effective treatment requires both wound care and correction of faulty veins. With early diagnosis, advanced vascular procedures, and structured follow-up, patients can achieve complete healing and significantly improve their quality of life.
If you are experiencing persistent leg wounds or symptoms of vein disease, timely evaluation can make a crucial difference in restoring skin health and overall well-being.